Table of Contents
- How TRT Covered by Insurance Actually Works
- TRT Medical Necessity: What Insurers Actually Require
- Types of TRT Covered by Insurance: A Breakdown
- Medicare and Medicaid Coverage for TRT in 2026
- Private Insurance and TRT: Blue Cross Blue Shield and Beyond
- TRT Insurance Pre-Authorization: A Step-by-Step Guide
- TRT Insurance Denial Appeal: How to Fight Back
- Cost of TRT Covered by Insurance vs. Paying Out of Pocket
- Alternative Payment Options When Insurance Won’t Cover TRT
- How Telemedicine Platforms Fit Into TRT Coverage
- Factors That Affect Whether TRT Is Covered by Insurance
- Conclusion
Last Updated: April 14, 2026
Testosterone prescriptions in the U.S. increased from 7.3 million in 2019 to over 11 million in 2024, and the question of whether TRT covered by insurance is achievable has become one of the most searched health finance topics for men navigating hormone therapy. This guide from Ascend Vitality breaks down exactly how coverage works, what insurers actually require, and how to fight back when your claim gets denied. The landscape is more navigable than most patients realize, but only if you understand the rules before you walk into your doctor’s office.
How TRT Covered by Insurance Actually Works
Getting TRT covered by insurance is not a matter of luck. It follows a predictable logic rooted in medical necessity, documentation, and your plan’s formulary, and understanding that logic is the difference between a covered prescription and a four-figure out-of-pocket bill.
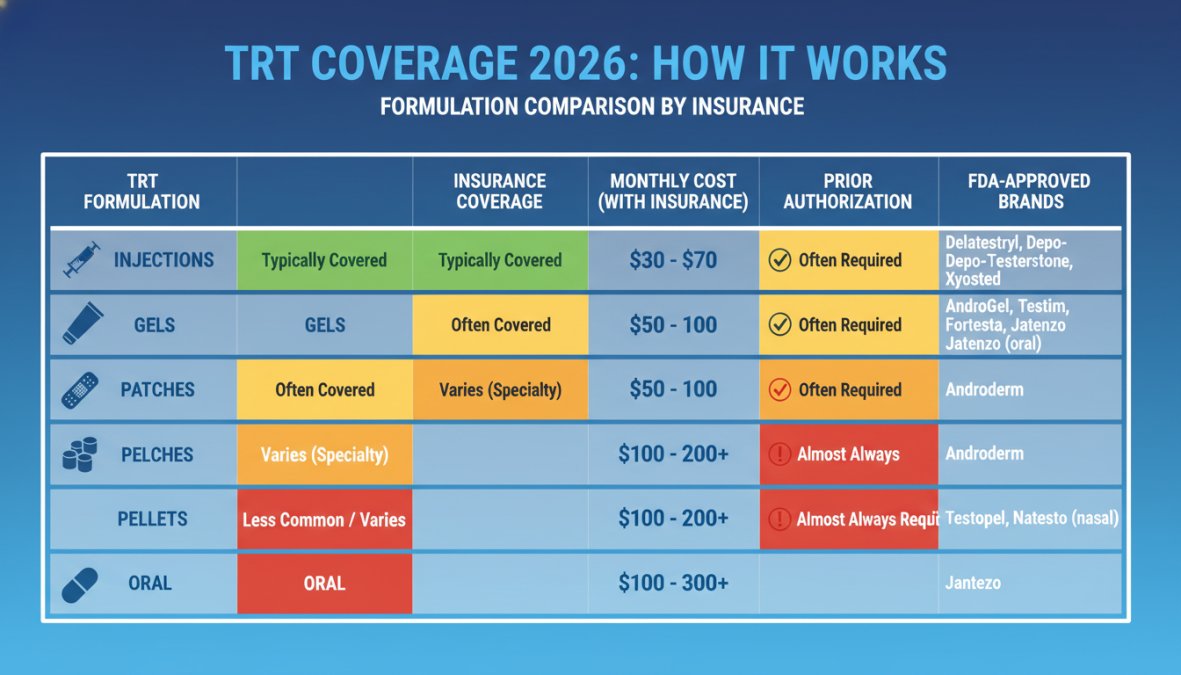

Insurance coverage for Testosterone Replacement Therapy is the process by which a health plan agrees to pay for some or all of the cost of testosterone treatment when a licensed physician documents a clinical diagnosis of hypogonadism or low testosterone. Coverage is not automatic. It requires a diagnosis, laboratory results, and in most cases, prior authorization.
The Role of Diagnosis and Laboratory Results
Your insurer does not take your word for it. The coverage process begins with blood tests, typically measured in nanograms per deciliter (ng/dL), that establish your testosterone levels against a clinical threshold. According to Highland Longevity (2026), most insurers require testosterone levels below 300 ng/dL combined with the presence of documented symptoms to approve TRT coverage.
That second part matters as much as the number. Symptoms such as fatigue, low libido, erectile dysfunction, loss of muscle mass, weight gain, reduced bone density, and difficulty with concentration must be documented in your medical record. A single low lab reading without a symptom picture is often insufficient. Your physician needs to connect the laboratory results to your clinical presentation before the insurer will move forward.
How Insurance Plans Evaluate Your Claim
Once your healthcare provider submits a claim or prior authorization request, the insurer runs it through their medical necessity review process. The reviewer checks three things: whether your diagnosis meets their clinical criteria, whether the specific drug formulation you were prescribed appears on their formulary, and whether you have tried any required prior treatments (a practice called step therapy).
Several factors affect whether insurance coverage is approved, including the type of insurance plan you carry, your testosterone levels relative to the plan’s threshold, and the specific TRT treatment your physician selected. Newer formulations like enclomiphene or oral testosterone may require additional prior authorization or may not yet appear on a plan’s formulary at all.
TRT Medical Necessity: What Insurers Actually Require
Most guides stop at "get your testosterone tested." That’s not enough. TRT medical necessity is a clinical and administrative standard, not just a lab result, and insurers apply it with varying degrees of strictness depending on the plan.
TRT medical necessity is the documented clinical justification that a physician provides to demonstrate that Testosterone Replacement Therapy is required to treat a diagnosed condition, specifically hypogonadism, rather than being elective or lifestyle-driven.
Symptoms That Support a Medical Necessity Claim
The symptoms your physician documents carry significant weight. Insurers are looking for a pattern consistent with hypogonadism, not isolated complaints. The most commonly accepted symptom clusters include:
- Persistent fatigue not explained by other conditions
- Decreased libido and sexual dysfunction, including erectile dysfunction
- Loss of muscle mass or strength despite regular activity
- Increased body fat or unexplained weight gain
- Reduced bone density confirmed by imaging
- Cognitive symptoms such as poor concentration or low mood
A common mistake is presenting only one or two symptoms. A well-documented medical necessity claim lists the full clinical picture, ties it to the laboratory results, and explains why other causes have been ruled out.
Documentation Your Physician Needs to Provide
Your physician’s documentation package is the backbone of any TRT medical necessity claim. At minimum, it should include:
- Two separate blood tests confirming low testosterone levels, taken on different days and ideally in the morning when levels peak
- A complete symptom history with onset dates
- Records ruling out secondary causes of low testosterone (pituitary issues, medication side effects, obesity-related suppression)
- A proposed treatment plan specifying the drug formulation, dosage, and monitoring schedule
- Any relevant specialist notes, particularly from endocrinology or urology
The thing nobody tells you about TRT insurance claims is that the second blood test is often the one that gets skipped. One reading is not enough for most plans. Two morning readings below 300 ng/dL, separated by at least a week, is the standard that satisfies most clinical review criteria.
Submitting a prior authorization with only one testosterone reading is the single most common reason initial requests are delayed or denied. Insurers interpret a single data point as insufficient evidence of sustained hypogonadism. Always confirm two separate blood tests are in the file before submitting.
Types of TRT Covered by Insurance: A Breakdown
Not all testosterone formulations receive equal treatment from insurers. The type of TRT your physician prescribes directly affects whether it will be covered, how much prior authorization scrutiny it faces, and what your co-pay looks like.
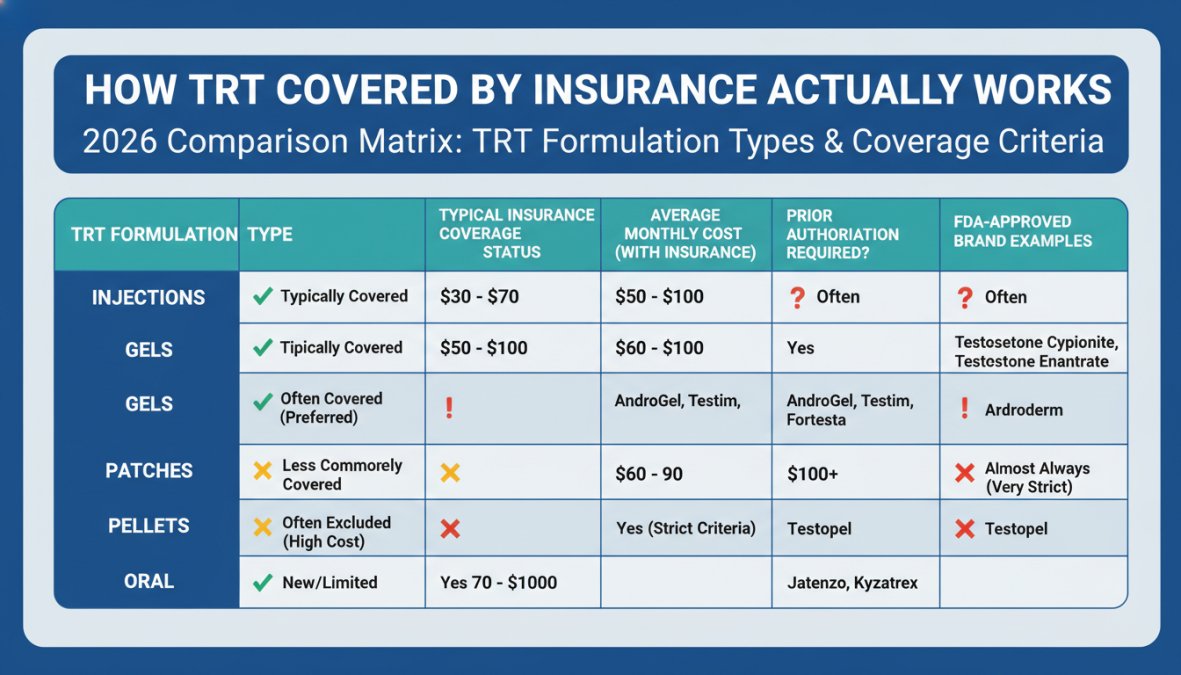
Generic Injections vs. Brand-Name Formulations
Generic injectable testosterone, specifically testosterone cypionate (Depo-Testosterone) and testosterone enanthate (Delatestryl), represents the most commonly covered TRT formulation. These are FDA-approved, widely available, and appear on most insurance formularies at the lowest tier, which means the lowest co-pay.
Brand-name injectable options like Aveed (testosterone undecanoate) occupy a different position. Aveed requires administration in a clinical setting due to the risk of pulmonary oil microembolism, which means it falls under medical benefit coverage rather than pharmacy benefit coverage. That distinction matters because the co-insurance calculation, deductible application, and prior authorization pathway are entirely different.
The practical upshot: if your physician starts you on generic injections, your path to coverage is straightforward. If they prescribe a brand-name formulation, expect additional steps.
Gels, Patches, Pellets, and Newer Oral Options
Testosterone gels and patches (topical formulations) are generally covered by insurance but tend to sit at a higher formulary tier than generics, meaning higher co-pays. They are FDA-approved and widely prescribed, so they clear medical necessity review without unusual friction.
Pellets, such as Testopel, are a different story. Many insurance plans classify subcutaneous pellet implantation as a procedure rather than a prescription, routing it through the medical benefit rather than the pharmacy benefit. Coverage varies significantly by plan, and some plans exclude pellets entirely.
Newer oral testosterone options face the steepest coverage challenges. Oral formulations are relatively recent FDA approvals, and many plans have not yet incorporated them into their formularies. Prior authorization is almost always required, and some plans will deny coverage pending longer-term safety data.
| TRT Formulation | Typical Coverage Status | Prior Auth Required | FDA Approved |
|---|---|---|---|
| Generic injections (Depo-Testosterone, Delatestryl) | Commonly covered, lowest tier | Sometimes | Yes |
| Testosterone gels/patches | Usually covered, mid-tier | Often | Yes |
| Aveed (injectable, brand) | Covered under medical benefit | Yes | Yes |
| Testopel (pellets) | Variable, plan-dependent | Usually | Yes |
| Oral testosterone | Limited coverage, newer option | Almost always | Yes (select brands) |
Medicare and Medicaid Coverage for TRT in 2026
Medicare and Medicaid operate under different frameworks than private insurance, and the rules for TRT coverage under each program are specific enough to warrant their own analysis.

Medicare Part B and Part D: What Each Covers
Medicare Part B covers TRT when administered by medical professionals in outpatient settings, such as physician-administered injections. According to data published in January 2026, Medicare Part B covers 80% of approved TRT costs after the deductible, with patients responsible for 20% coinsurance. This applies to formulations like Aveed that require clinical administration.
Medicare Part D covers self-administered TRT medications, including injections patients give themselves at home, topical gels, patches, and oral forms, based on the individual plan’s formulary and tier system. The 2025 Part D out-of-pocket cap of $2,000 carries forward into 2026, which provides meaningful protection for patients on long-term hormone therapy.
Medicare Advantage plans add another layer. Out-of-pocket limits for Medicare Advantage plans are $9,350 in-network and $14,000 combined in 2025, carrying into 2026. Patients comparing Medicare Advantage plans should specifically check how each plan handles TRT under both the medical and pharmacy benefit.
If you are on Medicare and your physician prescribes self-administered testosterone injections, ask whether the plan covers both the medication under Part D AND the injection supplies (syringes, needles) under Part B. Many patients miss the supply coverage and pay out of pocket for items that are technically reimbursable.
Medicaid Coverage: State-by-State Variability
Medicaid coverage for TRT is where the picture becomes genuinely complicated. Federal Medicaid rules establish a floor, but states have significant discretion in how they structure their formularies and medical necessity criteria. Some states cover a broad range of testosterone formulations with minimal prior authorization friction. Others restrict coverage to generic injections only, require specialist referrals before coverage begins, or impose step therapy requirements that delay access by months.
The practical advice here is direct: do not assume your state’s Medicaid program covers TRT the same way a neighboring state does. Call the member services number on your Medicaid card, ask specifically about testosterone replacement therapy coverage, and request the formulary document in writing before your physician submits a prescription.
Private Insurance and TRT: Blue Cross Blue Shield and Beyond
Private insurance coverage for TRT follows the same medical necessity framework as Medicare, but plan-to-plan variation is substantial. Blue Cross Blue Shield, as one of the largest private insurers in the United States, generally covers TRT when medical necessity is documented and the prescribed formulation appears on the plan’s formulary. However, Blue Cross Blue Shield operates through regional affiliates, and coverage policies differ between BCBS of Texas, BCBS of Illinois, BCBS of North Carolina, and other regional entities.
The most important thing to understand about private insurance and TRT covered by insurance is that your employer’s specific plan document governs what is covered, not the insurer’s general policy. An employer can negotiate a benefits package that includes or excludes specific drug categories. Some employer plans explicitly exclude testosterone therapy for conditions related to aging (sometimes called "age-related hypogonadism") while covering the same therapy for younger men with primary hypogonadism. This distinction is legally permissible and more common than most patients expect.
What most reviews of TRT insurance coverage miss is the role of the plan’s clinical policy bulletin. Every major insurer publishes these internally, and many make them available to members on request. The bulletin specifies the exact diagnostic codes, lab thresholds, and documentation requirements that trigger coverage approval. Getting a copy of your insurer’s clinical policy bulletin for testosterone replacement therapy before your physician submits a prior authorization request is one of the highest-use steps you can take.
Highland Longevity guide on TRT insurance coverage requirements
TRT Insurance Pre-Authorization: A Step-by-Step Guide
Prior authorization is the gatekeeper between a prescription and a covered medication, and TRT insurance pre-authorization is one of the more documentation-intensive examples in outpatient medicine. The good news: the process is predictable once you know what it requires.
What to Prepare Before Submitting Your Request
Before your physician’s office submits the prior authorization request, assemble the following:
- Two morning testosterone blood tests, taken on separate days, both below the plan’s threshold (commonly 300 ng/dL)
- A complete list of documented symptoms with onset dates in the physician’s notes
- The specific drug name, formulation, dosage, and route of administration your physician is prescribing
- The ICD-10 diagnosis code for hypogonadism (E29.1 for primary, E23.0 for secondary)
- Documentation ruling out secondary causes of low testosterone
- A copy of your insurer’s clinical policy bulletin for testosterone replacement therapy
- Your physician’s NPI number and practice information for the submission form
In practice, this means scheduling a pre-authorization prep appointment with your physician before they submit anything. Rushing the submission with incomplete documentation is the primary cause of delays.
Common Reasons Pre-Authorization Gets Delayed or Rejected
The most frequent reasons TRT insurance pre-authorization fails on the first submission:
- Only one testosterone blood test in the file
- Testosterone levels above the plan’s threshold (even if symptoms are present)
- Symptoms not documented in the physician’s notes prior to the authorization request
- Prescribed formulation not on the plan’s formulary
- Missing diagnosis code or incorrect ICD-10 code
- Physician’s notes written after the authorization submission date (a timing issue that creates credibility problems)
A common mistake is treating prior authorization as a formality. It is not. The medical reviewer assigned to your case is looking for specific clinical criteria, and if the file does not contain them, the request will be denied regardless of how symptomatic the patient actually is.
TRT insurance pre-authorization succeeds or fails on documentation quality, not on how symptomatic you are. A patient with severe hypogonadism who submits an incomplete file will be denied before a mildly symptomatic patient with a complete, well-organized submission.
TRT Insurance Denial Appeal: How to Fight Back
A denial is not a final answer. The TRT insurance denial appeal process exists precisely because initial reviews are often incomplete, and the appeals success rate for well-documented hormone therapy claims is meaningful.
Internal Appeals: Working Within Your Plan
The first step after a denial is the internal appeal. Your insurer is legally required to provide a written explanation of the denial, including the specific clinical criteria your claim failed to meet. Read that explanation carefully. It tells you exactly what to fix.
The internal appeal process for TRT insurance denial typically works as follows:
- Request the full denial letter with the specific criteria cited
- Have your physician write a letter of medical necessity that directly addresses each denial criterion
- Submit any missing documentation (second blood test, additional symptom records, specialist notes)
- Request a peer-to-peer review if available, where your physician speaks directly with the insurer’s medical reviewer
- Submit the appeal within the deadline specified in your denial letter (typically 30-180 days depending on the plan)
Peer-to-peer review is underused and often decisive. When a physician speaks directly with the insurer’s medical reviewer, the approval rate for initially denied TRT claims improves substantially. If your physician’s office does not proactively offer this, ask for it specifically.
External Review and Your Legal Rights as a Patient
If the internal appeal fails, you have the right to request an external review under the Affordable Care Act. An independent review organization (IRO), not affiliated with your insurer, evaluates whether the denial was clinically appropriate. The insurer is legally bound by the IRO’s decision.
External review is a meaningful protection. The ACA requires insurers to provide access to external review for most coverage denials, and the process is typically free for the patient. Your denial letter must include information about how to request external review. If it does not, contact your state insurance commissioner’s office.
U.S. Department of Labor guide on health plan appeals and external review rights
Cost of TRT Covered by Insurance vs. Paying Out of Pocket
Here’s where the financial picture gets genuinely interesting. The difference between insured and uninsured TRT costs is large enough to shape treatment decisions, and the long-term analysis reveals dynamics that short-term comparisons miss.
Long-Term Cost Analysis: Insurance vs. Self-Pay
With insurance, the cost of TRT can range from approximately $30 to $100 per month depending on coverage terms, the specific formulation, and the plan’s co-pay structure. That figure covers the medication itself. It does not include the cost of required blood tests, physician visits, or any procedures associated with formulations like pellet implantation.
Without insurance, the cost picture shifts dramatically. Generic testosterone cypionate injections are among the least expensive TRT options when purchased out of pocket, but brand-name formulations, gels, and patches carry significantly higher retail prices. Add in the cost of quarterly blood monitoring, physician oversight, and any co-morbidity management, and the annual out-of-pocket cost for uninsured TRT can reach several thousand dollars.
The long-term calculus favors pursuing insurance coverage aggressively before defaulting to self-pay, even when the pre-authorization process is cumbersome. The administrative investment in a successful insurance claim pays for itself quickly.
Using HSA and FSA Accounts to Offset TRT Costs
Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA) are legitimate tools for managing TRT costs, whether or not your insurance covers the therapy. TRT prescribed by a licensed physician for a diagnosed medical condition qualifies as a medical expense under IRS rules, making it eligible for HSA and FSA reimbursement.
This matters most for patients whose plans cover TRT but carry high deductibles, and for patients who self-pay while pursuing an appeal. HSA contributions reduce taxable income, and FSA funds are available at the start of the plan year, which means you can use the full year’s contribution immediately if you face a large upfront TRT cost.
If you are self-paying for TRT while your appeal is in process, pay using your HSA or FSA card rather than a personal credit card. You receive the tax benefit immediately, and if your appeal succeeds and your insurer retroactively covers the expense, you can reimburse your HSA for the amount recovered.
Alternative Payment Options When Insurance Won’t Cover TRT
Some patients will not achieve coverage regardless of how well they document their case. Age-related hypogonadism exclusions, plan-specific formulary restrictions, and employer benefit decisions can create coverage gaps that appeals cannot resolve. In those situations, several alternatives reduce cost without abandoning medically supervised treatment.
Patient assistance programs offered by pharmaceutical manufacturers cover some brand-name TRT formulations for patients who meet income criteria. These programs are worth investigating for formulations like Aveed that carry high retail prices. Generic manufacturer discount programs and pharmacy discount cards (GoodRx and similar services) can reduce the cost of generic testosterone injections substantially at participating pharmacies.
Compounding pharmacies represent another option, though one that requires careful evaluation. Compounded testosterone is not FDA-approved as a finished product, and insurance plans do not cover compounded formulations. The cost may be lower than brand-name options, but the regulatory status means you are outside the standard quality assurance framework. This is a trade-off worth discussing explicitly with your physician.
FDA guidance on compounded drug products and patient safety
How Telemedicine Platforms Fit Into TRT Coverage
Telemedicine has changed the access equation for TRT significantly. From 2018 to 2022, TRT use increased by 120% among men aged 24 and younger and 86% among men aged 25 to 34, a trend driven in part by the expansion of online hormone therapy platforms that removed geographic barriers to care.
The coverage question for telemedicine-based TRT is more nuanced than it appears. Many private insurance plans now cover telemedicine consultations at the same rate as in-person visits, meaning a telemedicine physician can order the blood tests, document the diagnosis, and submit a prior authorization request through the same pathway as an in-person physician. The medication itself, once prescribed, is covered or denied based on the same formulary and medical necessity criteria regardless of whether the prescribing physician was seen in person or online.
Where telemedicine platforms diverge from traditional care is in their approach to patients who do not qualify for insurance coverage. Many platforms offer direct-pay programs that bundle physician oversight, prescription, and delivery into a monthly fee that bypasses the insurance system entirely. For patients whose insurance will not cover TRT, this model offers a structured, medically supervised alternative to navigating the coverage system indefinitely.
Ascend Vitality operates in this space, connecting patients with specialized care pathways for hormone health and delivering medically-supported programs and prescriptions directly. For men who have exhausted the insurance coverage pathway or who want to begin treatment while an appeal is in process, a platform like Ascend Vitality provides access to supervised care without requiring insurance approval as a prerequisite.
Factors That Affect Whether TRT Is Covered by Insurance
Pulling the threads together: whether TRT covered by insurance becomes a reality for any individual patient depends on a specific set of variables. Understanding them upfront prevents wasted time and misdirected effort.
The primary factors that determine TRT insurance coverage outcomes:
- Testosterone level relative to plan threshold: Most plans use 300 ng/dL as the clinical cutoff, though some plans set the threshold lower. A level of 310 ng/dL may be denied even if symptomatic.
- Type of insurance plan: Medicare, Medicaid, employer-sponsored private insurance, and marketplace plans each operate under different rules. Medicare Part B and Part D have distinct coverage pathways for different TRT formulations.
- Specific drug formulation prescribed: Generic injections are the most consistently covered. Brand-name, pellet, and newer oral formulations face more scrutiny.
- Formulary placement: A medication on the formulary at Tier 1 costs far less than the same medication at Tier 3, even when both are technically "covered."
- Prior authorization requirements: Some plans require prior authorization for all TRT; others only for specific formulations or above certain dosage thresholds.
- Employer plan design: Employer-sponsored plans can exclude specific conditions or drug categories. Age-related hypogonadism exclusions are a known issue in some employer plans.
- Documentation quality: The completeness and clinical coherence of the physician’s submission is the single most controllable variable in the process.
The TRT market is projected to reach $1.13 billion by 2030, with North America holding a 36% share of the global market as of 2023. That growth reflects both rising diagnosis rates and expanding treatment options, but it also means insurers are paying closer attention to TRT claims than they were a decade ago. The coverage environment is not getting more permissive. Getting TRT covered by insurance in 2026 requires the same rigor it always has, applied more carefully than ever.
Testosterone Replacement Therapy Market forecast and growth analysis
Navigating TRT insurance coverage is genuinely complex, and the gap between a well-documented claim and a denied one often comes down to preparation rather than clinical eligibility. Ascend Vitality connects patients with specialized care pathways for hormone health, offering medically-supported programs with prescriptions delivered directly, so treatment does not have to wait on administrative timelines. For men who want structured, supervised hormone care with or without insurance approval, get started with Ascend Vitality and access the clinical oversight your treatment plan requires.
Frequently Asked Questions
What testosterone level do I need to qualify for TRT covered by insurance?
Most insurers require testosterone levels below 300 ng/dL combined with documented symptoms such as fatigue, low libido, erectile dysfunction, or reduced muscle mass before approving TRT coverage. Blood tests alone are often not sufficient, your healthcare provider must also document a clinical diagnosis of hypogonadism. Some plans may set different thresholds, so reviewing your specific policy's medical necessity criteria is essential before submitting a claim.
What are the most common reasons for a TRT insurance denial?
Common reasons for TRT insurance denial include testosterone levels above the plan's threshold, insufficient symptom documentation, failure to obtain prior authorization, or the prescribed drug formulation not appearing on the plan's formulary. Newer treatments like oral testosterone or enclomiphene may be denied more frequently as they often require additional prior authorization. Reviewing the denial letter carefully is the first step toward a successful TRT insurance denial appeal.
How do I appeal a TRT insurance denial?
Start by requesting the specific reason for the denial in writing. Gather supporting documentation, including laboratory results, your physician's notes, and evidence of symptoms. Submit an internal appeal within your insurer's deadline, typically 30 to 180 days. If the internal appeal fails, you have the right to request an external independent review under the Affordable Care Act. Having your healthcare provider write a letter of medical necessity significantly strengthens your TRT insurance denial appeal.
Does Medicare cover TRT in 2026?
Yes. Medicare Part B covers TRT administered by medical professionals in outpatient settings, paying 80% of approved costs after the deductible, with patients covering 20% coinsurance. Medicare Part D covers self-administered TRT medications, including injections, topicals, and oral forms, subject to the plan's formulary and tier system. The 2025 Part D out-of-pocket cap of $2,000 carries forward into 2026, which can meaningfully limit annual medication costs for beneficiaries.
What types of TRT are most likely to be covered by insurance?
Generic injectable testosterone formulations such as Depo-Testosterone and Delatestryl are typically the most likely types of TRT covered by insurance due to their lower cost and long-standing FDA approval. Gels and patches are often covered but may require step therapy, proving that injections were tried first. Pellets like Testopel and brand-name options like Aveed may face more coverage restrictions. Newer oral testosterone and enclomiphene often require prior authorization or may not yet appear on a plan's formulary.
How much does TRT cost with insurance?
With insurance coverage in place, TRT typically costs between $30 and $100 per month depending on your co-pay, deductible, and the specific drug formulation prescribed. Generic injections tend to fall at the lower end of this range, while branded gels or patches may cost more even with coverage. Without insurance, monthly costs can climb significantly higher, making it worthwhile to pursue coverage through your plan or explore HSA and FSA accounts to manage out-of-pocket costs.




