Table of Contents
- Quick Comparison: Best PCOS Treatment Options at a Glance
- How We Evaluated These PCOS Treatments
- 1. Hormonal Birth Control: Best for Regulating the Menstrual Cycle
- 2. Metformin: Best for Insulin Resistance and Metabolic Health
- How Long Does Metformin Take to Work for PCOS?
- 3. Letrozole and Clomiphene: Best PCOS Treatment Options for Fertility
- 4. Anti-Androgens Like Spironolactone: Best for Hirsutism and Acne
- 5. GLP-1 Receptor Agonists: An Emerging Option for Weight and Metabolism
- Inositol for PCOS: Your Top Questions Answered
- PCOS Diet Plan Example: What to Eat and Why It Matters
- PCOS Lifestyle Changes Best Practices: Exercise, Sleep, and Stress
- Which PCOS Treatment Is Right for You? A Decision Framework
- Conclusion
Last Updated: April 18, 2026
According to Grand View Research PCOS Treatment Market Report 2024, the global PCOS treatment market reached USD 4.79 billion in 2024 and is projected to hit USD 9.72 billion by 2035. The best PCOS treatment options have never been more varied or more evidence-backed than they are right now. This guide from Ascend Vitality breaks down 10 clinically supported approaches, from first-line medications to emerging therapies, so you can match the right intervention to your specific symptoms and goals. The landscape has shifted considerably in 2026, and what worked as standard advice five years ago no longer reflects current clinical thinking.
TL;DR:
- For irregular cycles: hormonal birth control remains the most reliable first-line option
- For insulin resistance and metabolic health: Metformin is the clinical standard, though GLP-1 agonists are closing the gap fast
- For fertility: Letrozole has replaced clomiphene as the preferred first-line agent
- For hirsutism and acne: Spironolactone is the anti-androgen of choice
- For holistic management: lifestyle changes, inositol, and combination therapy are the fastest-growing treatment category
Quick Comparison: Best PCOS Treatment Options at a Glance
Polycystic Ovary Syndrome (PCOS) is a hormonal disorder affecting the ovaries, characterized by chronic anovulation, elevated androgens, and metabolic dysfunction that requires individualized treatment rather than a one-size-fits-all protocol.
The table below summarizes the best PCOS treatment options by goal, so you can orient quickly before reading the full breakdowns.
| Treatment | Primary Goal | Best For | Key Limitation |
|---|---|---|---|
| Hormonal Birth Control | Menstrual regulation | Irregular cycles, acne, hirsutism | Doesn’t address insulin resistance |
| Metformin | Insulin sensitivity | Metabolic PCOS, weight management | GI side effects; slow onset |
| Letrozole | Ovulation induction | Anovulatory infertility | Not suitable if pregnancy not desired |
| Clomiphene | Ovulation induction | Fertility (secondary option) | Lower birth rates vs. Letrozole |
| Spironolactone | Androgen reduction | Hirsutism, acne, hair thinning | Requires contraception concurrently |
| GLP-1 Receptor Agonists | Weight and metabolism | Metabolic PCOS, obesity comorbidity | Emerging; long-term PCOS data limited |
| Inositol | Insulin sensitivity, ovulation | Mild-moderate insulin resistance | Supplement, not pharmaceutical-grade |
| Mediterranean Diet | Inflammation, insulin | All PCOS types | Requires sustained dietary commitment |
| Exercise Programs | Metabolic health, stress | All PCOS types | Results depend on consistency |
| Combination Therapy | Holistic management | Complex or multi-symptom PCOS | Requires coordinated clinical oversight |

How We Evaluated These PCOS Treatments
Every treatment on this list was evaluated against four criteria: clinical evidence quality, symptom specificity (what it actually addresses), practical accessibility, and risk-to-benefit profile. The 2023 international evidence-based guideline, highlighted in a March 2026 review published via Medscape Reference clinical review on PCOS management, confirms that PCOS management should be individualized, beginning with lifestyle modification and escalating based on symptom burden. That framework shaped how this list is ordered and framed.
What most PCOS guides get wrong is treating every patient as metabolically identical. PCOS presents in subtypes: lean PCOS, insulin-resistant PCOS, inflammatory PCOS, and adrenal PCOS each respond differently to the same interventions. The evaluations below flag which subtype each treatment suits best.
1. Hormonal Birth Control: Best for Regulating the Menstrual Cycle
Hormonal birth control is the most widely prescribed treatment for PCOS-related menstrual disruption, and for good reason. Compound oral contraceptives suppress androgen production, regulate estrogen and progesterone cycling, and reduce the risk of endometrial cancer caused by unopposed estrogen from chronic anovulation.
Pills, Patches, Rings, and IUDs: What’s the Difference?
The delivery mechanism matters more than most prescribers acknowledge. Here’s how the main options compare for PCOS specifically:
- Combined oral contraceptives (pills): Contain both estrogen and progestin. Most studied for PCOS. Reduce free testosterone, improve acne and excess hair growth, and restore menstrual cycle regularity. Best first-line choice for most patients.
- Patch and vaginal ring: Deliver similar hormones to pills with comparable efficacy for PCOS symptom management. Useful for patients with pill adherence issues.
- Hormonal IUD (Mirena): Progestin-only, primarily local effect. Protects the uterine lining but does not meaningfully reduce systemic androgen levels or improve hirsutism. A common mistake is assuming all hormonal IUDs manage full PCOS symptom burden. They don’t.
- Copper IUD: Non-hormonal. No benefit for PCOS symptoms beyond contraception.
The real-world picture is more complicated than clinical trials suggest. One case study from the All-Party Parliamentary Group on PCOS documented a patient prescribed oral contraceptives and later the contraceptive injection who reported some relief from menstrual disruption but expressed concerns about relying on birth control indefinitely as her only management strategy. That concern is legitimate. Hormonal contraception manages symptoms but does not treat the underlying endocrine disorder.
Hormonal birth control does not address insulin resistance. Women with metabolic PCOS who rely solely on the pill may see symptom improvement while their underlying metabolic risk continues to progress. Pairing it with Metformin or lifestyle intervention is often clinically appropriate.
2. Metformin: Best for Insulin Resistance and Metabolic Health
Insulin resistance sits at the core of most PCOS cases, and Metformin remains the most prescribed diabetes medicine for addressing it. By drug class, the insulin-sensitizing agents segment accounted for the largest share of 36.0% of the PCOS treatment market in 2024 (Grand View Research, 2024), which reflects how central metabolic management has become to PCOS care.

Metformin works by reducing hepatic glucose production and improving peripheral insulin sensitivity, which in turn lowers circulating insulin levels. Lower insulin means less androgen stimulation from the ovaries, which is why Metformin can partially restore ovulation and menstrual cycle regularity even without directly targeting hormone levels.
How Long Does Metformin Take to Work for PCOS?
Metformin typically takes 3-6 months to produce measurable improvements in menstrual regularity and androgen levels for women with PCOS. Metabolic markers like fasting glucose and insulin sensitivity often improve within 4-8 weeks, but reproductive outcomes require longer treatment periods.
The most common mistake is stopping Metformin after 6-8 weeks because "nothing is happening." In practice, this means patients abandon a treatment that would have worked if given sufficient time. GI side effects (nausea, diarrhea) are the main reason for early discontinuation. Starting at a low dose and titrating up over 4 weeks reduces this significantly.
Extended-release Metformin (Metformin XR) produces substantially fewer GI side effects than immediate-release formulations at equivalent doses. If your provider prescribes standard Metformin and you experience significant nausea, ask specifically about the XR formulation before discontinuing.
3. Letrozole and Clomiphene: Best PCOS Treatment Options for Fertility
Fertility management commanded 54.88% of the PCOS treatment market share in 2025 (Mordor Intelligence, 2026), which tells you exactly how many women are seeking ovulation induction as their primary treatment goal.
Letrozole has replaced clomiphene citrate as the first-line treatment for anovulatory infertility in PCOS, and the clinical data behind that shift is compelling. A double-blind trial by Legro et al. involving 750 anovulatory women with PCOS found that birth rates for letrozole and clomiphene were 27.5% and 19.1%, respectively, across treatment periods of up to five cycles (Medscape Reference). That 8.4 percentage point difference is not trivial when you’re talking about live birth outcomes.
Letrozole, an aromatase inhibitor, works by temporarily lowering estrogen levels, which prompts the pituitary gland to release more FSH and stimulate follicle development. Clomiphene, a selective estrogen receptor modulator, blocks estrogen receptors at the hypothalamus to trigger a similar FSH surge. Both induce ovulation, but letrozole produces a more physiological hormonal environment with lower multiple pregnancy risk.
For women with PCOS who want to conceive, the clinical recommendation as of 2026 is clear: start with letrozole. Clomiphene remains an option when letrozole is unavailable or contraindicated, but it is no longer the preferred first-line agent.
4. Anti-Androgens Like Spironolactone: Best for Hirsutism and Acne
Elevated androgens are responsible for the most visible PCOS symptoms: hirsutism (excess hair growth on the face, chest, and abdomen), acne, and androgenic hair thinning. Anti-androgens like Spironolactone block androgen receptors at the target tissue level, reducing the downstream effects of excess testosterone regardless of how much is circulating.
Spironolactone at doses of 50-200mg daily is the most commonly prescribed anti-androgen for PCOS in the United States. Results for acne typically appear within 2-3 months. Hirsutism improvement takes longer because existing terminal hair must cycle out, meaning 6-12 months is a realistic timeline for meaningful change.
Here’s what most reviews miss: Spironolactone must be used with contraception because of teratogenic risk. This makes it a natural pairing with combined oral contraceptives, which also independently reduce androgen production. The combination delivers additive benefit for both hirsutism and acne.
For women who want cosmetic improvement beyond what medication can achieve, laser hair removal and electrolysis address existing hair mechanically. These approaches work best when paired with Spironolactone, which slows new hair growth and extends the duration between sessions.
5. GLP-1 Receptor Agonists: An Emerging Option for Weight and Metabolism
GLP-1 receptor agonists are the fastest-moving category in PCOS pharmacology right now. According to a February 2026 analysis cited by BioSpace life sciences industry news, GLP-1 receptor agonists are increasingly recognized as a pivotal therapeutic option for metabolic dysfunction in PCOS, inducing substantial body weight reduction (mean 5.9 kg) and significantly improving insulin sensitivity.
The combination therapy regimens segment is expected to grow at the fastest CAGR in the PCOS treatment market during the forecast period (Mordor Intelligence, 2026), and GLP-1 agonists are central to that trend. A 2025 study found that combining standard therapy with GLP-1 receptor agonists offers superior efficacy in improving both metabolic and hormonal outcomes compared to standard therapy alone.
What separates GLP-1 agonists from Metformin in the PCOS context is their effect on appetite regulation and body weight. For women with PCOS whose BMI is significantly elevated and who have not achieved adequate metabolic improvement with Metformin alone, GLP-1 agonists represent a meaningful escalation option.
The honest limitation: long-term reproductive and hormonal outcome data specific to PCOS remains limited. These are not yet first-line agents for PCOS, but they are increasingly appropriate as second-line therapy for metabolic PCOS, particularly when weight loss is a treatment priority.
GLP-1 receptor agonists are not a PCOS cure. They address the metabolic dimension effectively, but women with significant androgen excess or fertility goals will still need additional targeted therapy alongside them.
Inositol for PCOS: Your Top Questions Answered
Inositol is a naturally occurring compound that improves insulin sensitivity and supports ovarian function. For women with PCOS, myo-inositol (and the combined myo-inositol/D-chiro-inositol ratio) has become one of the most studied supplement-based interventions available.
Does inositol actually work for PCOS? Research shows myo-inositol supplementation can reduce free testosterone levels, improve menstrual cycle regularity, and support ovulation in women with insulin-resistant PCOS. A 12-week trial by Jamilian et al. found that soy isoflavone administration significantly improved markers of insulin resistance, hormonal status, triglycerides, and biomarkers of oxidative stress in women with PCOS (Medscape Reference), which parallels the mechanisms through which inositol operates.
How much inositol should I take for PCOS? The most studied dose is 4g of myo-inositol daily, often combined with 400mcg of D-chiro-inositol in a 40:1 ratio. Inositol supplements are widely available and typically cost $15-$40 per month, making them one of the most accessible PCOS treatment options.
Can inositol replace Metformin? For mild-to-moderate insulin resistance without significant metabolic comorbidities, inositol is a reasonable alternative. For more severe insulin resistance or when fertility is the primary goal, Metformin or pharmaceutical ovulation induction is more appropriate. The two can be used concurrently under medical supervision.
What are the side effects? Inositol is generally well-tolerated. Mild digestive upset at higher doses is the most reported issue. Unlike Metformin, it does not require a prescription or blood glucose monitoring.
PCOS Diet Plan Example: What to Eat and Why It Matters
Dietary intervention is the most underutilized tool in PCOS management. The 2023 international guideline explicitly states that PCOS management should begin with lifestyle modification, yet most clinical encounters default immediately to medication. The right PCOS diet plan example addresses insulin resistance, inflammation, and androgen excess simultaneously.
A practical PCOS diet plan example should prioritize:
- Low-glycemic carbohydrates: Oats, legumes, sweet potatoes, and whole grains over white bread, white rice, and sugary beverages
- Anti-inflammatory fats: Olive oil, avocado, fatty fish (salmon, sardines), and walnuts
- Lean protein at every meal: Helps stabilize blood glucose and reduces post-meal insulin spikes
- Non-starchy vegetables: Fill half the plate to increase fiber and micronutrient density
- Limit ultra-processed foods: Processed foods drive insulin spikes and systemic inflammation, both of which worsen PCOS symptoms
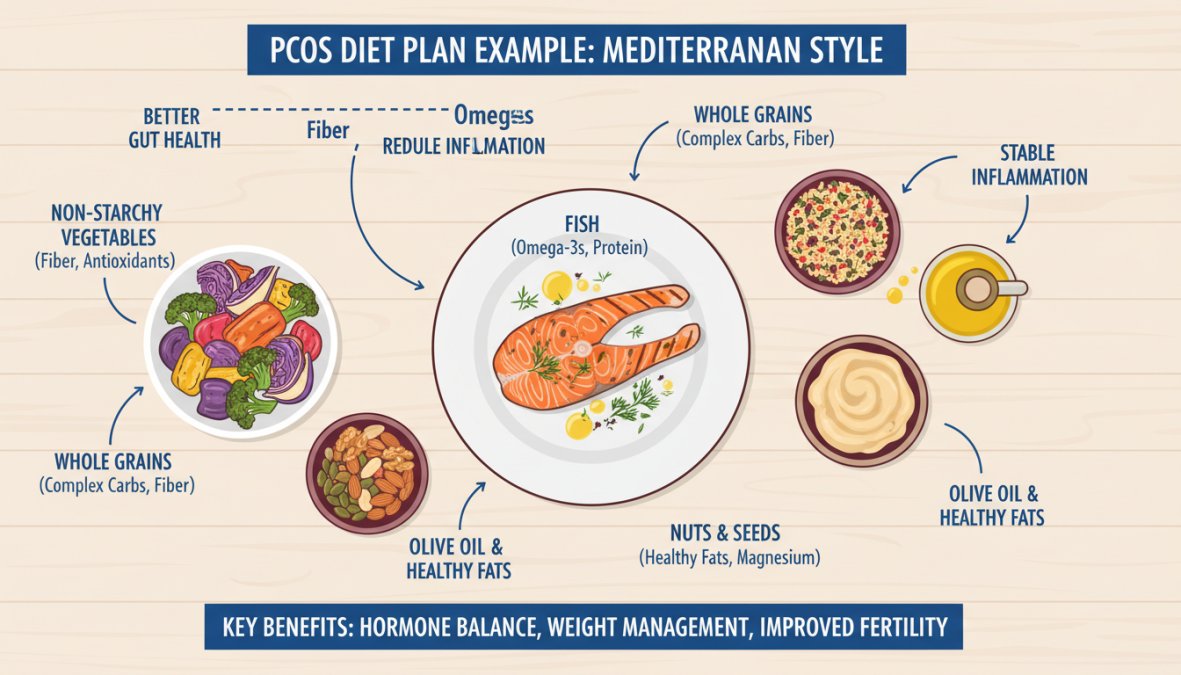
Mediterranean Diet as a Foundation
The Mediterranean diet is the most evidence-supported dietary pattern for PCOS management. It emphasizes whole grains, non-starchy vegetables, legumes, healthy fats, and lean protein, while limiting refined carbohydrates and processed foods. For women with PCOS, this pattern reduces insulin resistance, lowers systemic inflammation, and supports healthy weight management without requiring calorie restriction as the primary mechanism.
Working with a registered dietitian or nutritionist who understands PCOS-specific metabolic patterns is worth the investment. Generic low-calorie advice often misses the glycemic load dimension that matters most for insulin-resistant PCOS.
A contrarian point worth making: weight loss alone is not sufficient for most PCOS symptoms. A meta-analysis of 12 studies with 1,529 participants found that weight loss interventions can reduce insulin resistance and improve menstrual frequency, but may not significantly reduce hirsutism or improve quality of life (Medscape Reference, 2026). Diet matters for metabolic reasons, not just BMI reduction.
PCOS Lifestyle Changes Best Practices: Exercise, Sleep, and Stress
Exercise is one of the few interventions that simultaneously improves insulin sensitivity, reduces androgens, supports weight management, and lowers cortisol. The PCOS lifestyle changes best practices framework should treat physical activity as a clinical intervention, not an optional add-on.

The most effective exercise approach for PCOS combines three modalities:
- Moderate-intensity cardio (150 min/week): Walking, cycling, swimming. Improves insulin sensitivity and cardiovascular health.
- Resistance training (2-3x/week): Increases lean muscle mass, which improves glucose uptake independent of weight loss.
- Stress-reduction movement (yoga, Pilates): Lowers cortisol, which directly influences androgen production via the adrenal pathway. Particularly relevant for adrenal PCOS.
Sleep quality is the most overlooked lifestyle variable in PCOS. Poor sleep elevates cortisol and insulin, both of which worsen the hormonal environment. Women with PCOS have higher rates of sleep apnea and sleep disruption than the general population. Addressing sleep is not optional self-care; it is a clinical priority.
Chronic stress activates the HPA axis, driving adrenal androgen production. Stress management practices including mindfulness, adequate rest, and boundary-setting around work and social obligations are legitimate PCOS lifestyle changes best practices, not wellness platitudes.
Which PCOS Treatment Is Right for You? A Decision Framework
The best PCOS treatment options depend entirely on your dominant symptom cluster and primary treatment goal. This framework maps the most common presentations to the most appropriate starting point.
Decision Framework: Match Your Goal to Your First-Line Treatment
| Primary Goal | Dominant Symptom | First-Line Recommendation | Add-On to Consider |
|---|---|---|---|
| Regulate menstrual cycle | Irregular periods | Combined oral contraceptive | Metformin (if insulin resistant) |
| Improve fertility | Anovulation | Letrozole (aromatase inhibitor) | Metformin, lifestyle changes |
| Reduce hirsutism/acne | Excess androgens | Spironolactone + OCP | Laser hair removal |
| Manage weight/metabolism | Insulin resistance | Metformin or GLP-1 agonist | Mediterranean diet, exercise |
| Holistic management | Multiple symptoms | Combination therapy | Inositol, dietitian support |
| Minimize medication | Mild symptoms | Lifestyle modification | Inositol, spearmint tea |
Personalized medicine is becoming an important trend in the PCOS treatment market, with doctors moving toward treatments tailored to each patient’s genetic profile, metabolic status, and hormone levels (BioSpace, 2025). AI-enhanced ultrasound machines are now used to evaluate pelvic health, counting follicles and detecting structural changes with greater precision, leading to faster and more accurate diagnoses.
The practical implication: if your current provider is offering you a single medication without discussing your subtype, metabolic profile, or lifestyle factors, you are likely receiving incomplete care. A full diagnostic workup should include a pelvic exam, ultrasound, blood tests for hormone levels, and a glucose tolerance test before any treatment is finalized.
For women seeking accessible, medically supported pathways to PCOS treatment without navigating fragmented specialist referrals, Ascend Vitality offers targeted online care for weight loss, hormones, and metabolic health, with prescriptions and programs delivered directly to patients. The platform is built for exactly the kind of individualized, multi-symptom management that PCOS requires.
Women with multi-symptom PCOS who want a structured, medically supervised approach combining pharmaceutical support, metabolic management, and lifestyle guidance rather than a single-drug prescription.
One emerging area the best PCOS treatment options conversation rarely covers adequately: mental health. Anxiety and depression rates are significantly elevated in women with PCOS, and the bidirectional relationship between cortisol dysregulation and ovarian function means that untreated psychological stress actively worsens hormonal outcomes. Screening for mental health comorbidities should be part of any comprehensive PCOS evaluation.
Stem cell therapy represents the frontier end of PCOS treatment research. According to a case study documented in PubMed Central peer-reviewed research, intravenous and subdermal injections of umbilical cord-derived mesenchymal stem cells (UC-MSCs) in one patient completely resolved a 14-year history of menstrual irregularities and hormonal imbalances, with disappearance of ovarian cysts and sustained improvements for over a year. This is experimental, not clinical standard, but it signals where the field is heading.
The global PCOS treatment market is projected to reach USD 9.72 billion by 2035 (Polycystic Ovary Syndrome Treatment Market Size and Companies, 2026), driven by combination therapies, personalized medicine, and the growing recognition that PCOS is a lifelong endocrine disorder requiring sustained management rather than episodic treatment.
Managing PCOS effectively requires matching the right treatment to the right symptom profile, and that rarely means a single prescription. Ascend Vitality provides targeted online care for weight loss, hormones, and metabolic health, connecting patients with medically supported programs and prescriptions delivered directly to them. For women navigating multi-symptom PCOS without easy access to specialist care, get started with Ascend Vitality and access the individualized hormonal and metabolic support your treatment plan actually requires.
Frequently Asked Questions
What is the first-line treatment for PCOS?
According to the 2023 international evidence-based guideline, PCOS management should be individualized and begin with lifestyle modification, including diet, exercise, and weight management. For women not seeking pregnancy, hormonal birth control is commonly added to regulate the menstrual cycle and reduce androgen-related symptoms like acne and hirsutism. Metformin is often introduced when insulin resistance is a primary concern. The best PCOS treatment options depend heavily on your specific symptoms and health goals.
How long does metformin take to work for PCOS?
Most women begin to notice improvements in insulin sensitivity and menstrual regularity within 3 to 6 months of consistent metformin use. Some metabolic markers may improve sooner, but ovulation restoration and cycle regulation typically take longer. Metformin is often used alongside lifestyle changes for better results. Always follow your prescriber's dosing guidance, as starting at a low dose and titrating up helps reduce common gastrointestinal side effects like nausea and diarrhea.
What are good supplements for PCOS, and does inositol actually help?
Inositol, particularly myo-inositol, is one of the most researched supplements for PCOS. It can improve insulin sensitivity, reduce free testosterone levels, and support more regular menstrual cycles. Berberine is another option that may offer similar benefits to metformin for some women. Research by Jamilian et al. found that soy isoflavones taken for 12 weeks significantly improved insulin resistance markers and hormonal status in women with PCOS. Always discuss supplements with a healthcare provider before starting.
Is letrozole or clomiphene better for PCOS-related infertility?
Current evidence strongly favors letrozole. A double-blind trial by Legro et al. involving 750 anovulatory women with PCOS found live birth rates of 27.5% for letrozole versus 19.1% for clomiphene over up to five treatment cycles. As a result, letrozole has replaced clomiphene as the first-line treatment for anovulatory infertility in PCOS. Both are fertility treatments that stimulate ovulation, but letrozole's superior birth rates make it the preferred choice among reproductive specialists today.
Can PCOS be managed naturally without medication?
Lifestyle changes are a cornerstone of PCOS management and can meaningfully improve symptoms without medication for some women. A meta-analysis of 12 studies with 1,529 participants found that weight loss interventions can reduce insulin resistance, lower the free androgen index, and improve menstrual frequency. However, the same analysis noted that weight loss may not significantly reduce hirsutism or improve quality of life on its own. Natural approaches like the Mediterranean diet, regular exercise, inositol, and spearmint tea can complement, but often work best alongside, medical care.




